Champions for Children Giveathon benefiting Arkansas Children's Northwest expansion is today! GIVE NOW!
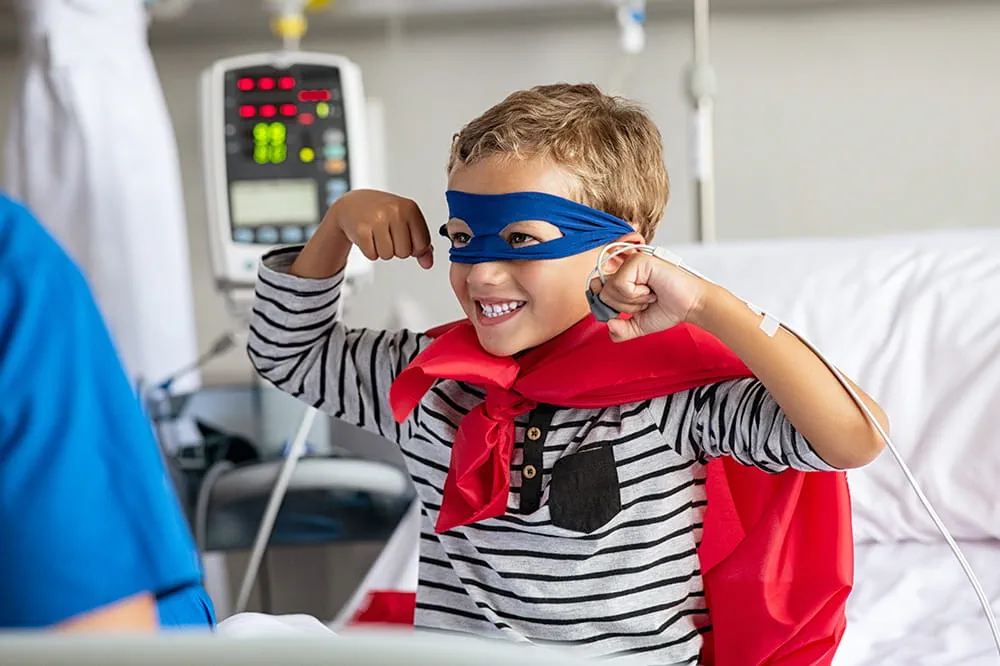
Ranked nationally in pediatric care.
Arkansas Children's provides right-sized care for your child. U.S. News & World Report has ranked Arkansas Children's in seven specialties for 2025-2026.

It's easier than ever to sign up for MyChart.
Sign up online to quickly and easily manage your child's medical information and connect with us whenever you need.
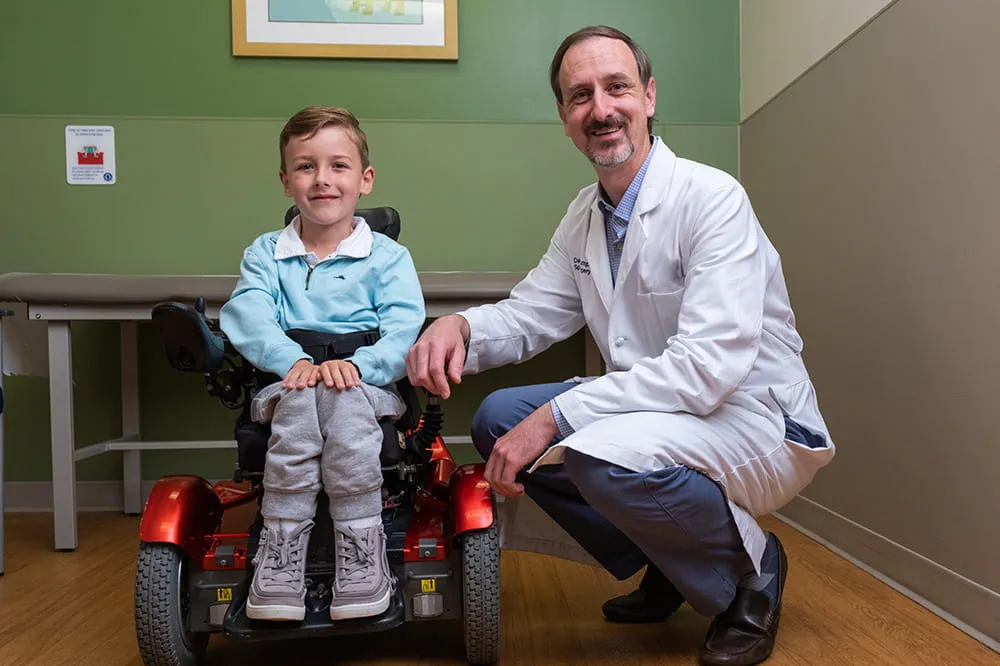
We're focused on improving child health through exceptional patient care, groundbreaking research, continuing education, and outreach and prevention.

When it comes to your child, every emergency is a big deal.
Our ERs are staffed 24/7 with doctors, nurses and staff who know kids best – all trained to deliver right-sized care for your child in a safe environment.

Arkansas Children's provides right-sized care for your child. U.S. News & World Report has ranked Arkansas Children's in seven specialties for 2025-2026.

Looking for resources for your family?
Find health tips, patient stories, and news you can use to champion children.

Support from the comfort of your home.
Our flu resources and education information help parents and families provide effective care at home.

Children are at the center of everything we do.
We are dedicated to caring for children, allowing us to uniquely shape the landscape of pediatric care in Arkansas.

Transforming discovery to care.
Our researchers are driven by their limitless curiosity to discover new and better ways to make these children better today and healthier tomorrow.

We're focused on improving child health through exceptional patient care, groundbreaking research, continuing education, and outreach and prevention.
Then we're looking for you! Work at a place where you can change lives...including your own.

When you give to Arkansas Children's, you help deliver on our promise of a better today and a healthier tomorrow for the children of Arkansas and beyond

Become a volunteer at Arkansas Children's.
The gift of time is one of the most precious gifts you can give. You can make a difference in the life of a sick child.

Join our Grassroots Organization
Support and participate in this advocacy effort on behalf of Arkansas’ youth and our organization.

Learn How We Transform Discovery to Care
Scientific discoveries lead us to new and better ways to care for children.

Learn How We Transform Discovery to Care
Scientific discoveries lead us to new and better ways to care for children.

Learn How We Transform Discovery to Care
Scientific discoveries lead us to new and better ways to care for children.

Learn How We Transform Discovery to Care
Scientific discoveries lead us to new and better ways to care for children.

Learn How We Transform Discovery to Care
Scientific discoveries lead us to new and better ways to care for children.

Learn How We Transform Discovery to Care
Scientific discoveries lead us to new and better ways to care for children.
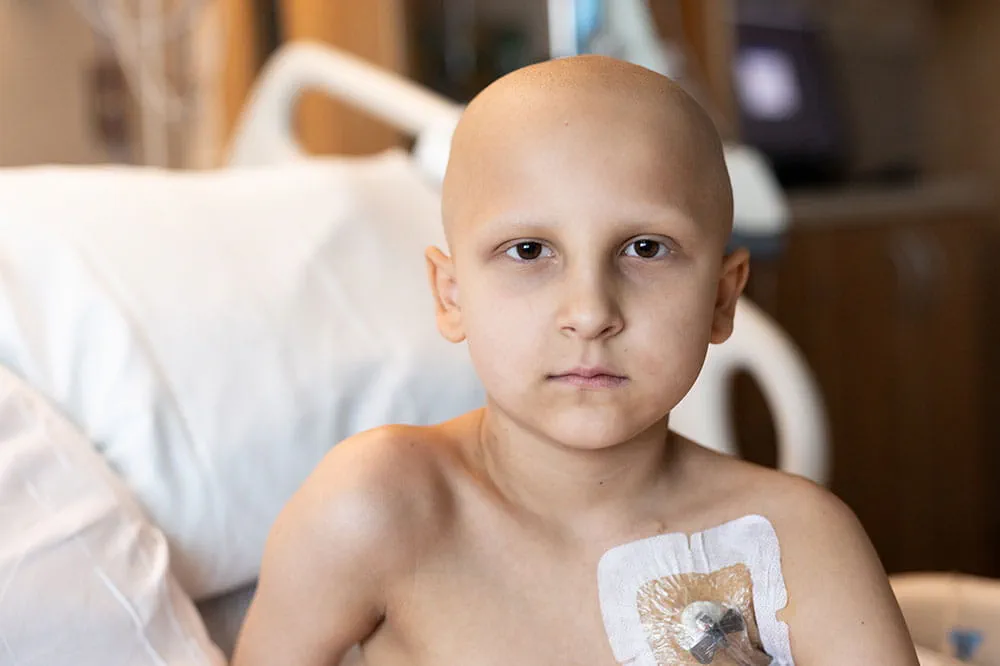
When you give to Arkansas Children’s, you help deliver on our promise of a better today and a healthier tomorrow for the children of Arkansas and beyond.

Your volunteer efforts are very important to Arkansas Children's. Consider additional ways to help our patients and families.

Join one of our volunteer groups.
There are many ways to get involved to champion children statewide.

Make a positive impact on children through philanthropy.
The generosity of our supporters allows Arkansas Children's to deliver on our promise of making children better today and a healthier tomorrow.

Read and watch heart-warming, inspirational stories from the patients of Arkansas Children’s.

Hello.

Arkansas Children's Hospital
General Information 501-364-1100
Arkansas Children's Northwest
General Information 479-725-6800

Summer Science Program

Photo: Summer Science Program Particpants 2025
The Summer Science Program at Arkansas Children's Hospital in Little Rock, co sponsored by the UAMS Department of Pediatricss and Arkansas Children's Research Institute, is intended to provide outstanding rising sophomore through senior level college students with a deep and focused experience in health-related research project under the guidance of active pediatric health-focused scientists. Research opportunities include laboratory-based experiences in basic and translational biology, clinical investigation, and community-based research projects. Student scholars will spend eight weeks during their summer primarily engaged in a mentored research project, with additional opportunities for touring hospital units and research facilities as well as shadowing physicians and researchers in rounds and clinics.
The Summer Science Program hosts a lecture series for participants highlighting elements of biomedical research including research methodology, introductions to academic pediatrics, and sessions exploring post-graduate educational pathways such as graduate school, medical school and other post-baccalaureate training. Student scholars will present the findings of their research projects to other program participants, mentors, and the Arkansas Children’s research community at the conclusion of the program.
The Summer Science Program offers valuable experience for college students interested in pursuing post-graduate training in biomedical sciences through an M.D., Ph.D., or M.D./Ph.D. program. A competitive stipend is offered to program participants. Limited housing is available, but the costs are not included in stipend support.
2026 Summer Science Program: June 1, 2026- Jul 24, 2026
Application Deadline: January 15, 2026
Notifications: Mid-February to the beginning of March
Eligibility Criteria
- Must be a full-time college student at the sophomore to senior level, not graduating before the 2026-2027 school year.
- Must provide application, recommendation letter, video interview, and transcript by the requested deadline.
- Must be a US resident or have a current US visa, as we can not sponsor visas for this purpose.

Summer Science Program Application
Apply
